7 Common Menstrual Disorders: Causes, Symptoms, and When to Seek Help
7 Common Menstrual Disorders: Causes, Symptoms, and When to Seek Help
Millions of women deal with period problems every month. Some brush it off as "just bad cramps." Others spend days in bed, missing work or school, quietly wondering if what they're feeling is actually normal.
Here's what most women aren't told: menstrual disorders are incredibly common, but common doesn't mean you have to live with them. Understanding your overall female health is the first step toward getting real help. This guide breaks down the 7 most common menstrual disorders in plain language so you can recognize what's going on and know when to do something about it.
What Are Menstrual Disorders?
A menstrual disorder is any condition that disrupts the normal pattern of your menstrual cycle. That includes changes in timing, how heavy your flow is, how much pain you feel, or emotional symptoms that show up around your period.
What Does a Normal Menstrual Cycle Look Like?
A healthy cycle runs somewhere between 21 and 35 days. Periods usually last 2 to 7 days. Soaking through one pad or tampon every 1 to 2 hours is considered normal. Anything that consistently falls outside those ranges deserves attention, especially if it keeps happening month after month.
7 Types of Menstrual Disorders You Should Know
1. Premenstrual Syndrome (PMS)

PMS is the most common menstrual disorder, affecting up to 75% of menstruating women. It's that familiar wave of physical and emotional symptoms that arrives in the one to two weeks before your period and fades once bleeding begins.
For most women, symptoms are annoying but manageable. For others, PMS is disruptive enough to affect relationships, work performance, and quality of life in ways that are hard to explain to people who haven't experienced it.
What Causes PMS?
Honestly, the exact cause still isn't fully understood, which is frustrating given how many women deal with it. What researchers do know is that PMS is tied to hormonal shifts in estrogen and progesterone during the second half of the menstrual cycle, along with changes in brain chemicals like serotonin. Symptoms disappear during pregnancy and after menopause, which points directly to the hormonal connection.
Common PMS Symptoms
On the physical side, expect bloating, breast tenderness, headaches, fatigue, joint pain, and acne flare-ups. Emotionally, mood swings, irritability, anxiety, food cravings, trouble sleeping, and difficulty concentrating are all common. The combination looks different for every woman, which is part of why PMS can feel so hard to pin down.
When Should You See a Doctor for PMS?
If symptoms are regularly affecting your work, relationships, and daily routine, have an honest conversation with your doctor. Severe or worsening PMS symptoms can sometimes be a sign of PMDD, which needs a different level of care.
2. Premenstrual Dysphoric Disorder (PMDD)
How Is PMDD Different From PMS?
Think of PMDD as PMS on a completely different level. Where PMS causes discomfort, PMDD causes real disruption. The emotional symptoms are far more intense and can make it genuinely hard to get through the day, hold down a job, or maintain relationships without everything feeling like a struggle.

What Causes PMDD?
Like PMS, PMDD is rooted in hormonal sensitivity and serotonin fluctuations. Some women are simply more reactive to the hormonal changes that happen mid-cycle. There's also likely a genetic component, and women with a personal or family history of mood disorders tend to be at higher risk.
PMDD Symptoms to Watch For
Severe depression or hopelessness, intense anger or irritability, panic attacks, feeling completely overwhelmed, extreme fatigue, difficulty concentrating, and noticeable appetite changes. The physical symptoms look similar to PMS. What sets PMDD apart is the severity and the way it takes over. Symptoms peak the week before your period and usually lift within a few days of bleeding starting, which can feel like a relentless monthly cycle with no real relief.
When to Seek Help for PMDD
If PMDD symptoms are seriously disrupting your life, don't put off getting help. If you're experiencing thoughts of self-harm, reach out immediately. PMDD typically requires a combination of therapy, medication, or hormonal treatment. Lifestyle changes help, but they usually aren't enough on their own, and recognizing that isn't a failure.
3. Dysmenorrhea: What Causes Painful Periods?
Dysmenorrhea is the medical term for painful menstrual cramps. It's the leading cause of missed school and work days among young women, which says a lot about how much it actually affects daily life. If you've ever had cramps so severe you couldn't get off the couch, you don't need a definition.

Primary vs Secondary Dysmenorrhea
Primary dysmenorrhea has no underlying condition behind it. The pain comes from high levels of prostaglandins, hormone-like chemicals that cause the uterus to contract strongly. It usually starts 1 to 3 days before your period and peaks around day one or two.
Secondary dysmenorrhea is driven by another condition such as endometriosis, uterine fibroids, adenomyosis, or pelvic inflammatory disease. It tends to get worse over time and often develops later in life, which is one reason it gets overlooked for so long.
Dysmenorrhea Symptoms
Intense lower abdominal cramping, pain that radiates into the lower back or thighs, nausea, vomiting, diarrhea, headache, and dizziness. When it's bad, it's genuinely debilitating.
When Period Pain Is Not Normal
Cramps that disrupt your life every single month, keep getting worse over time, or appear suddenly and severely after age 25 are worth investigating. That's no longer just "bad cramps." Secondary dysmenorrhea in particular needs a proper look for an underlying condition driving the pain.
4. Amenorrhea: Why Has My Period Stopped?
Amenorrhea means your periods are absent. It's not a diagnosis on its own, but a sign that something else is going on inside the body that needs to be identified.
Primary vs Secondary Amenorrhea
Primary amenorrhea means no period has arrived by age 15.
Secondary amenorrhea means someone who previously had regular cycles has missed three or more in a row.
What Causes Amenorrhea?
Hormonal causes: PCOS, thyroid disorders, pituitary problems, premature ovarian insufficiency
Lifestyle-related causes: Extreme weight loss, eating disorders, over-exercising, chronic stress
Structural causes: Uterine scarring, missing reproductive organs, vaginal obstructions
Medications: Certain contraceptives and other medications
Depending on what's causing it, you might also notice milky nipple discharge, hair loss, headaches, vision changes, or excess facial hair alongside the missed periods.
When to See a Doctor for Missed Periods
Start by ruling out pregnancy. If that's not the cause and your periods are still absent, get evaluated sooner rather than later. This matters beyond just your reproductive system. Missing periods for an extended time without a known reason can affect long-term bone density and hormonal health in ways that become harder to reverse the longer they go unaddressed.
5. Menorrhagia: How Heavy Is Too Heavy?

Menorrhagia means abnormally heavy or prolonged menstrual bleeding. A lot of women spend years assuming their heavy flow is just how their body works. Sometimes that's true. Often it isn't, and the good news is it's treatable.
What Causes Heavy Menstrual Bleeding?
Hormonal imbalances, uterine fibroids or polyps, adenomyosis, thyroid problems, bleeding disorders like von Willebrand disease, certain IUDs, pregnancy complications, and in rare cases, cancer.
Signs You May Have Menorrhagia
Soaking through one or more pads or tampons every hour for several hours in a row
Needing double protection or getting up at night to change protection
Passing blood clots larger than a quarter
Bleeding that goes beyond 7 days
Fatigue, dizziness, or shortness of breath from ongoing blood loss
When Heavy Periods Need Medical Attention
If bleeding soaks through protection every hour for more than two hours straight, don't sit on that. Left untreated, menorrhagia can lead to iron-deficiency anemia, which brings its own exhausting set of symptoms including extreme fatigue, pale skin, and difficulty concentrating. Your body can only handle so much blood loss before it starts showing the strain.
6. PCOS: How Does It Affect Your Menstrual Cycle?
Polycystic ovary syndrome, or PCOS, is a hormonal disorder that affects 5 to 10% of women of reproductive age worldwide. It disrupts ovulation, which throws the entire menstrual cycle off balance and sets off a chain reaction of symptoms that extend well beyond just your period.
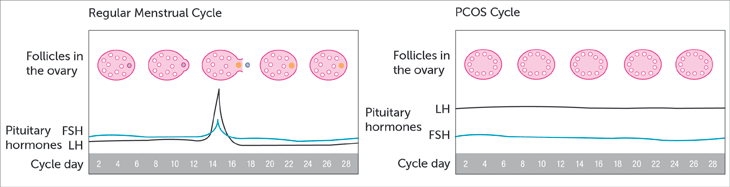
What Causes PCOS?
Insulin resistance, excess androgens (male hormones that exist in all women but are elevated in PCOS), low-grade inflammation, and genetics all contribute. Together they interfere with regular egg release, creating hormonal imbalance and irregular cycles.
PCOS Symptoms Related to Your Period
Fewer than 9 periods per year or cycles longer than 35 days apart
Very heavy or very light bleeding when periods do come
Difficulty conceiving because ovulation is irregular or absent
Additional signs include excess facial or body hair, severe acne, and thinning hair on the scalp
When to See a Doctor for PCOS
Irregular periods, signs of elevated androgens, or trouble getting pregnant are all good reasons to get evaluated. PCOS caught early means better long-term outcomes and a lower risk of developing type 2 diabetes, heart disease, and endometrial cancer down the line.
7. Endometriosis
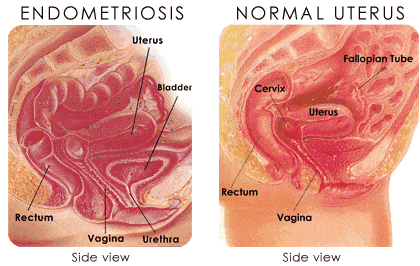
Endometriosis happens when tissue similar to the uterine lining grows outside the uterus, most often on the ovaries, fallopian tubes, or pelvic lining. That tissue responds to hormonal changes the same way it would inside the uterus, causing inflammation, internal bleeding, scarring, and serious pain.
It affects roughly 1 in 10 women of reproductive age in the United States and remains one of the most underdiagnosed conditions in women's health. The average time from first symptoms to an actual diagnosis is 7 to 10 years. That gap exists largely because severe period pain has been normalized for so long that many women don't realize their body is signaling something that genuinely needs attention.
What Causes Endometriosis?
The exact cause still isn't clear. Leading theories point to retrograde menstruation, where period blood flows backward into the pelvis rather than out of the body, immune system dysfunction that fails to clear misplaced tissue, and genetic factors.
Endometriosis Symptoms During Your Period
Severe period pain that starts before bleeding and lingers for days after it ends
Heavy periods or spotting between cycles
Pelvic pain during sex, bowel movements, or urination
Fatigue, bloating, and nausea that worsen around your period
When Endometriosis Needs Medical Evaluation
If your period pain is consistently worse than typical cramps, or it keeps intensifying over time rather than staying the same, that's your cue to speak with a doctor. Trouble conceiving is another reason to get evaluated. Endometriosis shows up in up to 50% of women with infertility, which makes early investigation worth it.
When to See a Doctor for Any Menstrual Disorder
You don't need to wait until things become unbearable. So many women are conditioned to push through period problems without ever asking whether something deeper is going on. But your cycle is one of the most reliable windows into your overall health. When something changes, your body is usually trying to get your attention.
Reach out to a healthcare provider if you notice:
Cycles shorter than 21 days or longer than 35 to 38 days
Bleeding that soaks through the protection every hour for several hours
Period pain that stops you from going about your normal day
Three or more missed periods with pregnancy ruled out
New or worsening symptoms after age 25
Signs of anemia, including dizziness, extreme fatigue, or pale skin
Spotting between periods or any bleeding after menopause
None of these are uncomfortable things to bring to your doctor. They're exactly what your gynecologist needs to know.
CONCLUSION
Period problems are common, but they are not something you have to just endure. Conditions like PMS, PMDD, painful or heavy periods, PCOS, and endometriosis all have real treatment options, from lifestyle changes to medical care.
The biggest challenge is often taking symptoms seriously after years of being told they are “normal.” But common does not mean normal, and you deserve better.
Track your cycle, notice patterns, and speak to a doctor who listens. Your reproductive health is an important part of your overall well-being.